As we become more active, our bodies become more susceptible to overuse and injury. In particular, our tendons, which are involved in muscle movement, are easily damaged. Tendons are the fibrous connective tissues that attach a bone to a muscle. Many movements involve pulling on a tendon for the desired muscle to contract.
Tendinopathy is the broad term for any disorder of the tendon, which includes tendinosis and tendonitis. It is commonly a result of overuse from repeated activity. While athletes are particularly at risk, ultimately, anybody can be affected. Those with hypertension, diabetes, obesity and high cholesterol are also at higher risk.
The amount we use our tendons reflects the ubiquity of the disorder. About 30 percent of clinical consultations for musculoskeletal pain are related to tendinopathy.1 With such a high prevalence, you, or someone you know, may be affected, so it’s important to educate yourself on the causes and treatments.

How does it occur?
When we injure a tendon, there is a cascade of biological processes that occurs to ensure it fully heals. Our body sends out signals, essentially waving its hands in the air calling for help. Ideally, these signals initiate blood to flow to that region (inflammation), “clean up cells” (macrophages) to remove damaged tissue, growth factors to regenerate the tissue, and collagen to proliferate in an organized manner. Collagen is the primary component of tendons and is essential to the proper functionality of the musculoskeletal system. In the case of tendinopathy, the healing process does not go as planned. Under the microscope, one might find less inflammatory cells, collagen degeneration and disorganization and hypercellularity (an excess of cells).2 Basically, the immune response is not responding to our body’s call for backup.
How is it treated?
We focus treatment on tricking the body into getting the proper response, one way or another. Standard conservative treatment options that apply to general musculoskeletal injury remain effective for tendinopathy. This includes ice/heat, activity modification, stretching, physical therapy, bracing and anti-inflammatory medication. These typical treatments generally resolve the pain, but sometimes further options need to be explored.
Several different types of injections can be favorable in treating tendinopathy. Platelet-rich plasma (PRP) has strong empirical support for alleviating tendon pain. The process takes advantage of using the patient’s own platelets and injecting them into the problem area. Platelets are beneficial as they accelerate cell growth and healing. Another type of injection is prolotherapy, which entails injecting an irritant such as dextrose around the area of pain. It sounds counterintuitive, but the irritant stimulates the immune response that leads to inflammation and healing. Finally, dry needling/fenestration is a technique that involves a needle puncture to instigate inflammation and, therefore, the healing response.
Nitroglycerin patches are another non-invasive choice that has had promising outcomes. Nitroglycerin produces nitric oxide, which stimulates collagen growth and vasodilates to increase blood flow. These patches have been shown to decrease pain, improve range of motion, and improve the muscular force.
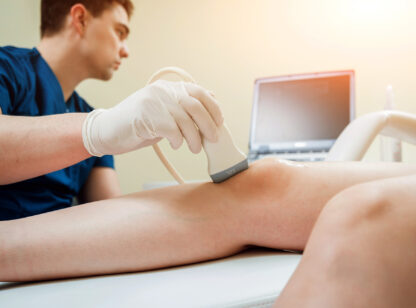
Wave therapy is an emerging treatment alternative that uses sound or light waves to treat the condition. Shockwave therapy involves a series of high energy sound waves directly applied to the area of concern. The pulses of waves lead to new blood vessel formation, decreased inflammation, and stimulus of collagen synthesis. Ultrasound therapy is another form of soundwave therapy that uses high frequency, low energy waves. The energy from the sound wave is converted to heat and increases local blood flow and tissue relaxation while decreasing scar tissue. Lightwave therapy involves lasers that use non-thermal photons through the skin at multiple wavelengths and depth to decrease pain, inflammation and edema.
When all options are exhausted, surgery may be the best solution for the patient. Skilled surgeons can repair the tissue in an operating room, however, it should be reserved as a last resort. In most cases, more conservative options are sufficient for reducing symptoms.
Since tendinopathy is so prevalent, it’s important to understand exactly what it is, how it happens, and how to treat it. Our bodies do what they can to ensure a smooth healing process, but they are not foolproof. The immune system’s failure to follow the correct steps of healing affects many people in the form of tendinopathy. Thankfully, there are many promising, non-invasive treatment options available today.
Founding physician Eric Sickinger, DO and medical assistant Thalie Timsit, BS are with Advanced Center for Sports & Musculoskeletal Medicine. For more information, contact their Palm Desert office at (760) 636.1067 or the San Clemente office at (949) 388.1060, or visit www.SportsandMSKmedicine.com.
References:
1) Lipman, Kelsey, et al. “Tendinopathy: Injury, Repair, and Current Exploration.” Drug Design, Development and Therapy, Volume 12, 2018, pp. 591–603.;
2) Sharma P, Maffulli N. Biology of tendon injury: healing, modeling and remodeling. J Musculoskelet Neuronal Interact. 2006;6(2):181-190.








































Comments (0)