One of the most common reasons people seek medical attention is due to back pain,1 and much of that pain originates in the lower back. While many suffer with short periods of acute pain, 23% of adults globally suffer from chronic low back pain (LBP) which lasts 12 or more weeks and is the leading cause of disability worldwide.2
The good news is that most LBP can be relieved with simple home remedies. Doctors agree this should always be the first course of action before heading to urgent care unless you have pain following a fall or blow to the back, new bowel/ bladder problems, or fever accompanying the pain, all symptoms that could signal a serious medical issue.1
“Barring any red flags like trauma or infection, the right thing to do for LBP is to start off conservatively: modify your daily activities, apply ice and take over-the-counter anti-inflammatories to see if that resolves,” says neurosurgeon Randall McCafferty, MD.
Physical therapy and manual manipulation by a chiropractor, osteopathic doctor or other qualified health professional can be the next step before seeking medications such as muscle relaxers or biologic injections from a primary care or pain management physician.
Diagnosing the cause. This can be challenging – even for the most skilled practitioners. “If symptoms progress and or continue after conservative measures are taken, then you may want to start seeking a diagnosis,” says McCafferty. “There is a lot of cross over in pain pathologies and factors to consider include location, precursors to pain, relieving factors, if the pain radiates and how, if there is numbness or weakness and more.” Patient history, a physical exam and diagnostic tests can help point your care team in the right direction, but they don’t always paint a clear picture, he says.
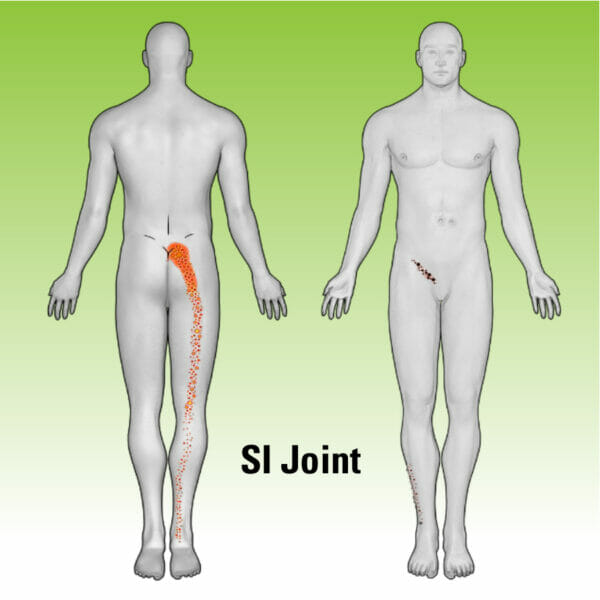
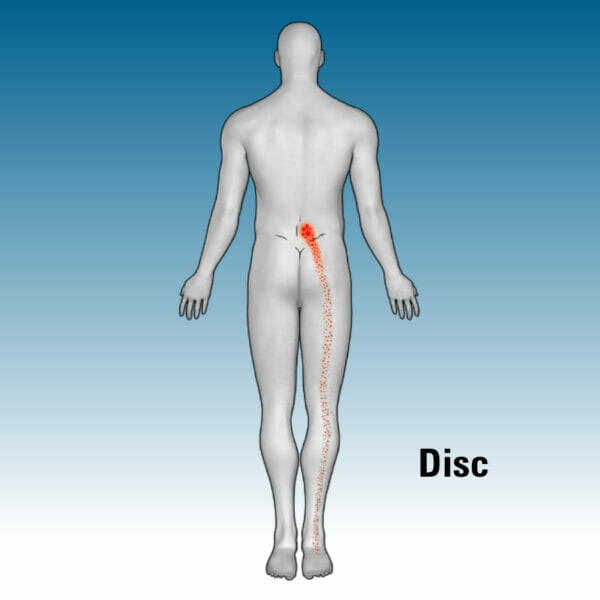
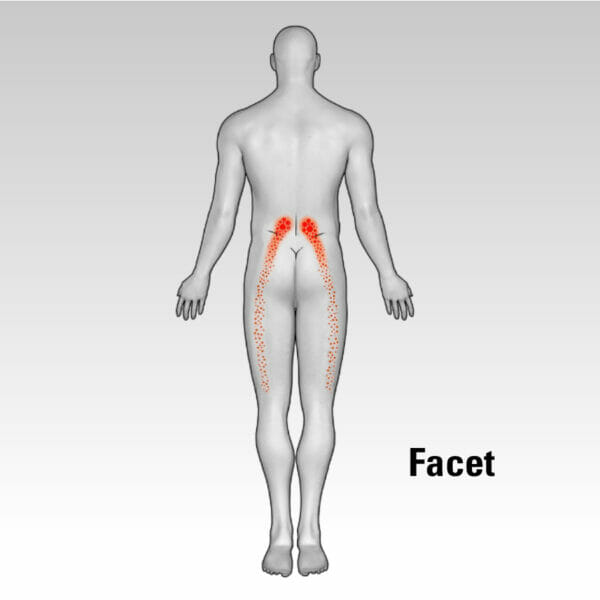
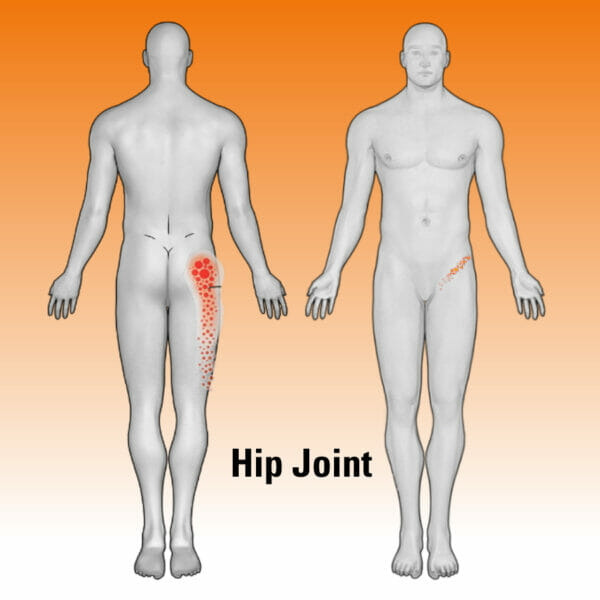
“I spend a lot of time listening to patients, and often they give you really good insights into what you should be looking for,” he adds. The diagrams shown here indicate common pain referral patterns to help patients and their care team identify the possible root cause: spinal disc degeneration, posterior spine joint dysfunction (facet), hip joint irregularities or possibly an area now more commonly considered, the sacroiliac (SI) joint which accounts for 15-30% of LBP cases.3
“It wasn’t until this past decade that we had viable options to treat SI joint dysfunction, so doctors didn’t standardly consider this area,” says McCafferty. He adds that there are now very good diagnostic guidelines and targeted therapies.
“SI joint dysfunction can be hard to identify as symptoms mirror other types of lower back pain,” agrees sports medicine physician Eric Sickinger, DO. “But in those cases I have treated, most resolve with targeted physical therapy.”
Causes of SI joint dysfunction. Like other joints, age degeneration and inflammation are significant factors, along with trauma such as a fall or vehicle accident which can create force on the SI joint, explains McCafferty. He adds that woman can also develop SI joint pain during pregnancy, and those who have had past back surgeries are at higher incident. “Patients who may have had a previously successful back surgery may later have recurring pain due to biomechanical strain on the SI Joint.”
McCafferty utilizes five manual manipulation tests he considers tell-tale signs of SI dysfunction. “If three of the five are positive and the historical intake leads me to believe this may be the cause of pain, my next course of action is a referral to a pain management doctor for an SI joint diagnostic block.”
The block is an anesthetic injection into the SI joint which should produce immediate relief. If that relief lasts for as long as anticipated based on the medication, it is consider a positive test.
Treating SI dysfunction. Like other LBP, SI joint dysfunction therapies start with the conservative methods mentioned above. From there, a common recommendation is radiofrequency ablation which damages or destroys the nerve causing pain. This therapy standardly offers substantial short-term relief (six months or so), says McCafferty, but with only 20% of patients maintaining relief at 12 months.
“There are many, many steps that lead to surgical intervention,” he adds. “It is not until all these steps are taken, and I have a thorough historical intake and positive diagnostic block that I begin introducing surgical options.”
At that point, the game-changing technology is a 3-D printed porous implant that bridges across the sacrum and iliac wing. “Unlike most fusions I do, where I am laying bone to get new bone growth to fuse joints, this technology leaves enough space for the bone to grow directly into the implant and fuse the joint.” The minimally-invasive procedure led by x-ray guidance immediately stabilizes the joint allowing it to fuse over time.
“We are seeing a 90% patient satisfaction with reduction in disability and pain,” says McCafferty.
Identifying SI joint pain. “I recommend patients consider what is medically referred to as the Fortin finger test,” concludes McCafferty. “If the origination of LBP pain is off-center of the spine midline – that boney area just a few centimeters right or left – that is reason for me to consider the SI joint.”
Lauren Del Sarto is founder/publisher of Desert Health and can be reached at
Lauren@DesertHealthNews.com.
References: 1) https://www.ninds.nih.gov/health-information/disorders/back-pain; 2) https://www.ncbi.nlm.nih.gov/books/NBK538173/; 3) https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8517984.






































Comments (0)