Neck pain is a frequently encountered problem in society. It is associated with a significant decrease in quality of life and a significant increase in time off work, which is associated with a decrease in national economic productivity.
Patients typically present to either their primary care doctor or the emergency room with complaints of moderate-to-severe neck pain, with or without arm pain. Neck pain can vary in location from midline to paraspinal in nature and can at times radiate to the back of the head. Patients can have severe sharp shooting pains down the arms to the fingers, as well as weakness of specific muscles of the arms. In severe cases, patients can present with weakness of the hands and legs and/or immobility.
Cause
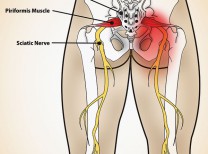
Causes of neck pain include traumatic injury, myofascial inflammation, and spinal disease. Traumatic injuries can result from falls, accidents, whiplash injuries, and acute acceleration and deceleration events. Myofascial inflammation is irritation of the fascia overlying the muscles due to a variety of causes such as whiplash injuries and fibromyalgia. Spinal disease includes cervical degenerative disc disease or arthritis affecting the vertebrae in the neck. Inflammation of the joints of the spine, nerve compression, and deformity of the vertebrae over time can cause significant neck pain and arm pain.
Careful history is critical in determining cause of pain , including the patient’s past medical history, prior surgeries, smoking history, family history, medications, allergies and other bodily complaints. A thorough physical examination of the entire body, including neurological testing of the arms and legs, is critical to identify areas of weakness, atrophy, or numbness localizing in a particular area of compression in the cervical spine.
Diagnosis
Diagnostic modalities to determine cause of neck pain include the following: CT scan of the cervical spine to identify bony deformity and arthritis; MRI of the cervical spine to identify spinal cord or nerve root compression; flexion extension x-rays of the cervical spine to determine instability; DEXA scan to determine bone density quality; and nuclear SPECT CT scans to determine areas of increased osteoblastic activity and bony remodeling.
Treatment
Treatments for myofascial disorders of the neck include acupuncture, physical therapy, aqua therapy, TENS units, massage, chiropractic treatment, pain management consultation for injections, and cervical traction. If no significant abnormalities are noted on the diagnostic tests in such patients, treatments are non-surgical in nature.
Initial treatment for cervical spine pathology include acupuncture, physical therapy, aqua therapy, TENS units (Transcutaneous Electrical Nerve Stimulation), massage, chiropractic treatment, pain management consultation for epidural steroid injections, and cervical traction. If such conservative measures do not work, surgical options come into play. If diagnostic studies demonstrate severe spinal cord compression from cervical disc herniation or abnormal movement of one vertebra over the other with deformity of the spine, surgical intervention is recommended for spinal cord and nerve root decompression and restoration of spinal structural stability.
Surgical intervention on the neck can be performed from an anterior, posterior or combined approach depending on what the diagnostic studies and patient symptoms/examination demonstrate. Patients with MRI evidence of anterior pathology such as disc herniation will be best treated with an anterior approach on the right side of the neck through a small 2-inch incision over a skin crease. This procedure is called an anterior cervical discectomy and fusion (ACDF) and allows for complete disc removal and nerve decompression followed by fusion of the selected vertebral levels. If the MRI demonstrates multiple levels of spinal cord compression from a predominantly posterior location, then a posterior approach to spinal cord and nerve root decompression is recommended. Such a procedure is called a posterior cervical decompression and fusion (PCDF) to allow for a complete and thorough neuronal decompression with stabilization of the selected vertebrae. In cases of both anterior and posterior pathology, with associated deformity or abnormal bending of the spine causing the chin to come closer to the chest, a combined anterior and posterior approach would likely be recommended.
Success rates are very high and patients can often return to work within 4 weeks to 3 months, depending on the type of procedure performed. Most simple anterior or posterior operations are associated with only 1-3 days of hospitalization.
Minimizing Risks
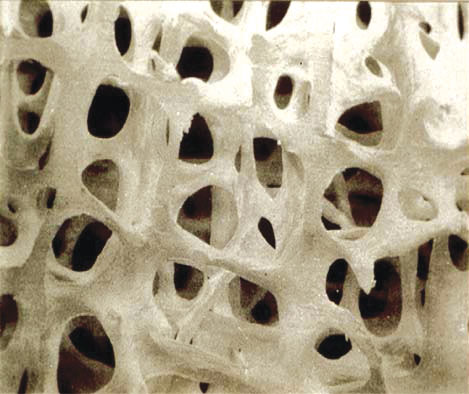
Smoking has been found to be associated with a weakening of, and increased degeneration of, the spine. Counseling for such patients in smoking cessation is recommended, especially in patients who are candidates for surgery, as smoking can affect wound healing and fusion rates. Additionally, bone density evaluations, hormone levels of parathyroid, estrogen, testosterone, and vitamin D should be routinely obtained in such patients to improve overall outcome.
All in all, neck pain is quite complex. However, utilizing and understanding the above paradigm will help patients heal and live life with significantly less discomfort.
Paul E. Kaloostian MD, FAANS, is board-certified in neurosurgery. He can be reached at (760) 346.8058 or at www.DrEtebar.com. He is also a member of Desert Doctors. For more information visit DesertDoctors.org or call (760) 232.4646.








































Comments (0)