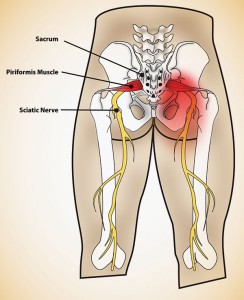
 The painful and irritating condition we commonly call “sciatica” is also known as sciatic neuritis, sciatic neuralgia, or lumbar radiculopathy. It involves one of five spinal nerve roots of the sciatic nerve which is the longest and widest single nerve in the body. It begins in the lumbar spine (lower back) from the spinal nerves L4 (L – Lumbar) through S3 (S – Sacral) and travels through the buttock and down the lower limb to the foot on both sides.
The painful and irritating condition we commonly call “sciatica” is also known as sciatic neuritis, sciatic neuralgia, or lumbar radiculopathy. It involves one of five spinal nerve roots of the sciatic nerve which is the longest and widest single nerve in the body. It begins in the lumbar spine (lower back) from the spinal nerves L4 (L – Lumbar) through S3 (S – Sacral) and travels through the buttock and down the lower limb to the foot on both sides.
Why is it so painful? Almost all of the skin of the leg, the muscles of the back of the thigh, the leg, and the foot are supplied by the sciatic nerve. If there is compression or irritation of one of the five spinal nerve roots, this can result in symptoms including low back pain, buttock pain, and pain, numbness or weakness in various parts of the leg or foot. One may also experience pins and needles or tingling and difficulty moving or controlling the leg. The pain from sciatica can be severe and debilitating for some, and less frequent and irritating to others, but with the potential of getting worse.
What Causes Sciatica?
The common causes of compression include:
Spinal disc bulge or spinal disc herniation (a herniated intervertebral disc)
Discs are like shock absorbers that cushion the spine from compression forces. The spinal discs consist of a fibrous tough ring of cartilage known as the annulus fibrosus with an egg yolk type liquid center, the nucleus pulposus. They separate the vertebrae allowing space for the exiting nerve roots coming from the spinal cord. The discs are weak when rotational pressure movements are applied to the spine – such as during a golf swing or lifting and twisting.
When the liquid center bulges in an outward direction (most commonly posterior lateral toward the spinal nerve roots), there is tearing of the annulus fibrosus, resulting in compression of the nerve root against an internal portion of the spinal vertebra, causing sciatica. Additional compression may develop due to inflammation and swelling of the surrounding tissues.
Spinal stenosis
Spinal stenosis is a narrowing of the spinal canal (the opening where the spinal cord runs) causing compression on the spinal cord or sciatic nerve roots. Stenosis of the foramina (the opening created by an arch at the top of one vertebra and an arch at the bottom of the vertebra above where the spinal nerve exits on either side) will also cause compression on the spinal nerve root exiting between these two vertebrae.
Spinal stenosis may be caused by inflammation, herniated disc, spondylolisthesis (a slipping of one vertebra on another), or a bone spur, resulting in a narrowing of the space, irritating and pinching the spinal nerves and creating sciatic pain.
Diagnosis
Sciatica is usually diagnosed by a physical examination and history of the symptoms. While tests may be positive in 90% of people with sciatica, approximately 75% with a positive test do not have sciatica.
Additional studies such as a CT or MRI may be recommended to diagnose a lumbar disc herniation.
Treatment
Medications
Medications are typically prescribed for sciatica to reduce swelling and relieve immediate pain; however, evidence for the effectiveness of analgesics is poor. Evidence is also lacking in the use of opioids and muscle relaxants which are often prescribed.
Spinal manipulation
There is moderate quality evidence that spinal manipulation (a chiropractic adjustment) is an effective and generally safe treatment for sciatica. Chiropractic adjustments provide joint mobilization helping to normalize joint motion aiding in reducing inflammation, swelling and nerve irritation.
Decompression Therapy
Axial spinal decompression has demonstrated an ability to significantly reduce intradiscal pressure to a negative 150mm Hg. allowing for disc decompression. Patients with sciatica and abnormal sensory function with positive examination and positive imaging studies reported an overall improvement of 67% after receiving spinal decompression therapy. Patients with disc involvement reported 86% relief of their symptoms after a course of axial spinal decompression therapy.
There are surgical options available for sciatica, but many of these procedures have been shown to only provide short term relief. The aforementioned are non-invasive therapies and should be considered prior to spinal surgery. Speak to a qualified health care practitioner to determine the best treatment for your condition.
Dr. Le Roy is a doctor of chiropractic and can be reached at 760.771.4800.
Sources: Valat, JP; Genevay, S; Marty, M; Rozenberg, S; Koes, B (2010 Apr). “Sciatica.”. Best practice & research. Clinical rheumatology 24 (2): 241–52; Mayo Clinic Guide To A Healthy Pregnancy Harms, Roger W., M.D., et al, Part 3.; Miller TA, White KP, Ross DC (September 2012). “The diagnosis and management of Piriformis Syndrome: myths and facts”. Can J Neurol Sci 39 (5): 577–83; Valat, JP; Genevay, S; Marty, M; Rozenberg, S; Koes, B (2010 Apr). “Sciatica.”. Best practice & research. Clinical rheumatology 24 (2): 241–52; Valat, JP; Genevay, S; Marty, M; Rozenberg, S; Koes, B (2010 Apr). “Sciatica.”. Best practice & research. Clinical rheumatology 24 (2): 241–52; Pinto, RZ; Maher, CG; Ferreira, ML; Ferreira, PH; Hancock, M; Oliveira, VC; McLachlan, AJ; Koes, B (2012 Feb 13). “Drugs for relief of pain in patients with sciatica: systematic review and meta-analysis.”. BMJ (Clinical research ed.) 344: e497; Waseem, Z; Boulias, C; Gordon, A; Ismail, F; Sheean, G; Furlan, AD (2011 Jan 19). “Botulinum toxin injections for low-back pain and sciatica.”. Cochrane database of systematic reviews (Online) (1): CD008257; Bruggeman, AJ; Decker, RC (2011 Feb). “Surgical treatment and outcomes of lumbar radiculopathy.”.Physical medicine and rehabilitation clinics of North America 22 (1): 161–77; Leininger, Brent; Bronfort, Gert; Evans, Roni; Reiter, Todd (2011). “Spinal Manipulation or Mobilization for Radiculopathy: A Systematic Review”. Physical Medicine and Rehabilitation Clinics of North America 22 (1): 105–125; F Tilaro; D Miskovich, “The effects of Vertebral Axial Decompression On Sensory Nerve Dysfunction”,Canadian Journal of Clinical Medicine, Vol 6, No1, Jan 1999; C. Norman Shealy, MD, PhD, and Vera Borgmeyer, RN, MA, “Decompression, Reduction, and Stabilization of the Lumbar Spine: a Cost-Effective Treatment for Lumbosacral Pain”, Am Journal of Pain Management Vol.7 No.2 April 1997.













































Comments (2)
Hello Iam muzaffar i have a disease like sciatica iam belongs to pakistan and residence of hyderabad sindh i ask my problem my left left legs back side is totally numbness from left hip to left foot and another thing my penis left side and also ball is paralyss so plz send me medicine name which is available in pakistan stores plz iam suffering from this deseas from 13 years i also checkup many more doctors plz help me send me on my email address muzaffaralilangah@yahoo.com
Dear Muzaffar Ali,
I recommend that you see your primary care doctor or a neurologist for you sciatic condition. They will be able to properly diagnose and treat you.
Best to you,
Lawrence Le Roy, DC