Light therapy, which is now referred to as photomedicine, has been utilized in ancient civilizations for over 3,000 years. One of the latest advancements is photodynamic therapy (PDT) which combines laser light with a photosensitizing agent (topical, oral or IV drug or supplement) to prepare the treatment area for greater light penetration. It was first utilized in 1978 to treat lung cancers in dogs, confirming the safety and efficacy of the treatment. In 1994, the first-generation infusion photosensitizer, Photofrin, gained approval for PDT use in Japan. Since 2003, 76 clinical trials have been registered in Europe, and PDT is now used worldwide to treat multiple types of cancers and chronic diseases.
In the United States, PDT is used primarily for dermatological treatments of actinic keratosis, acne and some skin cancers such as basal cell and squamous cell carcinoma. PDT can also relieve symptoms of esophageal and lung cancers that obstruct airways. The technology has also been used in trials for non-operable biliary, ovarian, bladder, breast and early prostate cancers. Other conditions PDT may help include arthritis and joint pain, acute infections, Lyme and other chronic infectious diseases, Alzheimer’s and mood disorders, to name a few. PDT also has anti-aging applications.
How does it work?
PDT utilizes a multidisciplinary approach, applying chemistry, physics and pharmacology to the clinical healing sphere. Using a photosensitizer prior to applying low-level lasers makes tumor tissues, or pathogens, more sensitive to the specific light waves applied. In the presence of oxygen, the photosensitized targeted tissues form reactive oxygen species (ROS) leading to apoptosis (cell death) and cellular immune modulation.
First- and second-generation FDA-approved photosensitizers include Photofrin (infusion), Levulan (topical) and Foscan (injection). Third-generation nanoparticles are being studied and developed for more targeted treatment. Other natural sources of photosensitizers can be taken orally or given via IV, such as Indocyanine green, chlorin E6, riboflavin, curcumin, Epigallocatechin gallate (EGCG) and hypericin. PDT can also be used in combination with photosensitizing chemotherapeutics, such as 5-FU, Xeloda (Capezitabine)- a 5-FU prodrug and Cisplatinin.
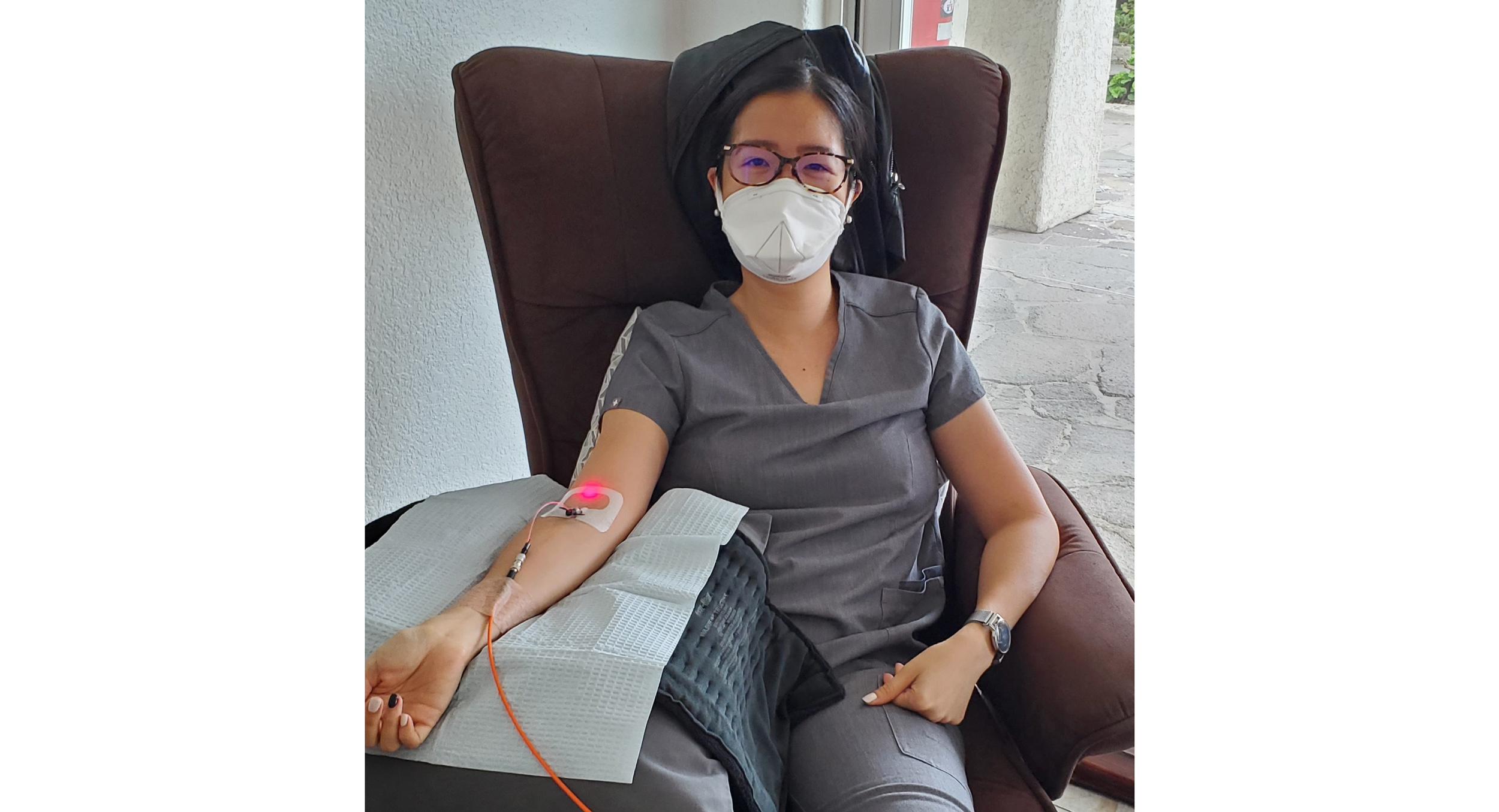
PDT applies light-emitting diodes (LED) with wavelengths mostly within the visible spectrum (380-800 nanometers). These lasers differ from sunlight or lamp light with their ability to emit one stable color. Treatment can be with one or more colors with a photosensitizer. PDT employs ultraviolet, green, blue, red, yellow and infrared lasers, each designed to provide distinctive benefits:
- Ultraviolet – Enhances oxygen absorption into targeted tissues while breaking down viral, fungal or bacterial presence.
- Blue – Enhances strong anti-inflammatory and antibacterial properties while promoting pain relief, wound recovery and anti-aging effects through activation of telomerase and mitochondria.
- Green – Improves oxygen uptake while decreasing discomfort caused by swelling or acute inflammation. Helps improve glucose metabolism.
- Yellow – Increases production of serotonin and vitamin D, providing antidepressant properties, as well as strong antibacterial, antiviral, and antiparasitic properties. It can be used for certain cancer therapies as well.
- Red – Provides energizing effects while strengthening immunity, increasing cellular activity and promoting wound healing. It can be used for certain cancer therapies as well.
- Infrared – Promotes wound healing, reduces pain and inflammation and increases mitochondrial production of ATP. IR has deepest penetrative power of the laser spectrum and can penetrate up to 7cm, thus utilized for neurological disease.
Before 2000, PDT was mostly limited to topical and superficial uses due to the limited penetration of light waves, even with a photosensitizing agent. However, newer technology allows for the insertion of fine fiber optic wires interstitially (within the tissue). Interstitial laser therapy was first utilized in 2003 by Vogl et al. in Frankfurt, Germany, to treat metastatic liver tumors. Intravenous laser therapy or “systemic PDT” was first introduced by Kaplan et al. in 2008 for the treatment of metastatic malignant melanoma. PDT is an in-office treatment (20-60 minutes), is minimally invasive and can be safely utilized concurrently with other cancer therapies, such as surgery, radiation therapy or chemotherapy.
One of the positive distinctions of PDT is its safety and low side effect profile. Common side effects are skin photosensitivity for three days up to six weeks depending on the area and transient localized tenderness. Topical PDT does not break the skin; however, the darker the skin type, the lower the intensity of the treatment and the increased number of treatments are needed to minimize damage to the dermal tissues.
Intravenous PDT utilizes an IV catheter, and interstitial PDT uses specialized guide needles that allow for the insertion of the fiber optic lines to the targeted area. Treatment length and intensity depend on the individual, the condition treated and the patient’s skin type.
Photodynamic therapy has shown remarkable potential for a broad scope of therapeutic effects ranging from anti-inflammatory, antimicrobial, to anti-tumoral. The majority of current clinical trials for PDT are for cancer, demonstrating its potential efficacy in oncology. As awareness of this low-risk therapy increases, PDT should become more available in outpatient clinics across the US.
Dr. Sonja Fung is a primary care naturopathic doctor with a focus on integrative cancer care and PRP regenerative joint injections. She is the founder and medical director at the Live Well Clinic in La Quinta which now offers photomedicine. For more information, call (760) 771.5970 or visit www.livewellclinic.org.
Sources available upon request.















































Comments (2)
Would this be an effective treatment for Granuloma Annulare?
Thank you, Shelley! I will reach out to Dr. Fung and I am sure she will get back to us promptly.
Thank you for reading Desert Health.
Lauren Del Sarto
Publisher