Editorial adapted from study published in American J Managed Care, July 2021.
Desert Medical Advances of Coachella Valley (DMA) is a rheumatology clinic specializing in clinical trials for the past 30 years. Recently, our team conducted a causal inference study using prospective data from 39 clinical trials globally compared to over a thousand patients locally that participated in the same 39 trials. The study concluded that patients in the Coachella Valley have shown less morbidity and mortality than age-matched patients in the rest of the world.
The reason? The local group received vaccination against infectious disease1 resulting in less illness, less hospitalization, less shingles, and less death. The vaccines were part of DMA’s preventative care program and donated to local subjects via clinical trials. Vaccines were not provided for the global trial sites.
In statistical multivariate analysis, we were able to show that vaccines were responsible for patient improvement. Other preventative measures included treatment for diabetes, hypertension and cholesterol, and while they showed numerical improvement in cardiovascular events, they were much less potent and take much longer to have an effect on morbidity and mortality. Vaccines showed efficacy within a year of use and are clearly essential in medical care.3
The subjects: 28,105 patients enrolled in 28 different clinical sites globally were compared to 1,088 patients in the Coachella Valley over an average five year span. Subjects were all rheumatoid arthritis (RA) patients from prospective randomized trials. This group was chosen because they are prone to infection and preventive care could influence outcomes.
Methods: Nested data from DMA were compared with global data in 39 pivotal studies using immune therapies for RA. Data were extracted from new drug applications (NDAs) submitted for FDA approval including tumor necrosis factor inhibitor (adalimumab, etanercept, certolizumab, and infliximab), Janus kinase inhibitor (tofacitinib, baricitinib, upadacitinib, and filgotinib), rituximab, abatacept, interleukin IL-1 (anakinra, canakinumab), and IL-6 (tocilizumab) therapy.
DMA participated in each study; entry criteria, age, concomitant medication, and intervention were identical. Safety results were gleaned from the FDA website2 and safety data included death from any cause. This evaluation explored death from major adverse cardiovascular events (MACE), pneumonia, and infections with zoster (shingles).
DMA instituted 10 specific preventive care measures including: 1) vaccination for influenza, pneumonia, and zoster; 2) hypertensive treatment for blood pressure greater than 140/90 mm Hg; 3) diabetes treatment if glycated hemoglobin A1C was greater than nine percent; 4) treatment for uric acid greater than 7 mg/dL; 5) statin therapy if low-density lipoprotein cholesterol was greater than 120 mg/dL; 6) diet intervention if body mass index was greater than 30, including a visit with staff dietitian every three months; 7) chewable aspirin 81 mg/day; 8) daily prenatal vitamin with 1 mg folate (given to all patients to ensure 1-mg folate dose necessary when taking methotrexate; 9) daily sinus wash (NeilMed) to decrease upper respiratory infection; and 10) no use of corticosteroids or narcotics.
Results (as demonstrated in Tables A and B):
- Less shingles. Shingles incidence decreased between 2005 and 2020. Key to this decline was Zostavax approval in 2006 and Shingrix approval in 2017. Locally, shingles vaccines for all started in 2006 and resulted in significantly less incidence compared to the global population.
- Less pneumonia and death due to infection. Pneumonia events were lower in the local subjects than the global population (P < .004). All local subjects had influenza and pneumonia vaccination. Deaths due to infection were also lower here (about one-third of deaths in all RA trials globally were due to pneumonia).
- Less mortality. A data subset of older patients (aged 63-70 years) with long-term follow-up of three to seven years showed all-cause mortality was less in these older subjects locally (0.3% vs 2.8%; P < .007).
- Less major adverse cardiovascular events for the older Coachella Valley population which was followed for three to seven years: 0.5% vs 0.9% (P = 0.3). Locally, treat-to-target for hypertension, cholesterol and diabetes, as well as, dietary classes for weight control and exercise were offered to all subjects.
- Fewer thrombotic events. Local subjects had fewer thrombotic events (blood clots) than those in the global studies (P < .03 in the longer follow-up trials); locally, all subjects took chewable aspirin 81 mg/d.
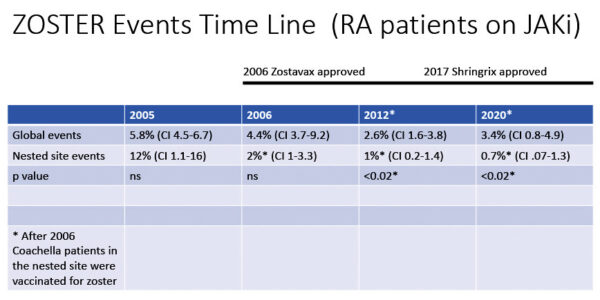
Table A 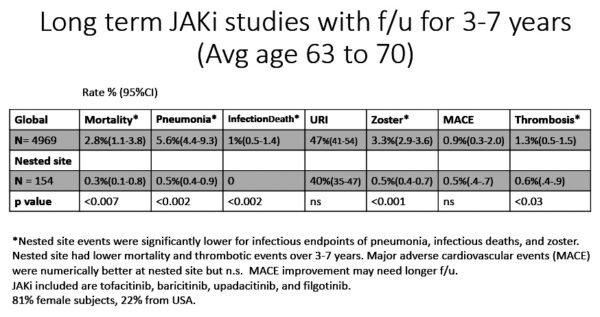
Table B
Our study clearly demonstrates that over the years, vaccines have helped save lives in the Coachella Valley. Prior to COVID-19 vaccine accessibility, our clinic lost six patients to the disease, many with young families who now live without them. Since receiving the vaccine on January 6, 2021, DMA has vaccinated all of our 2,200 patients. We have not had a single COVID related death or hospitalization since.
Dr. Greenwald is president and medical director of Desert Medical Advances of Coachella Valley. She is a member of Desert Doctors and can be reached at (760) 341.6800. Visit www.DesertDoctors.org.
Disclosures: 1) Author Affiliations: Desert Medical Advances (MoG, JB, SL, MB, MaG), Palm Desert, CA; 2) Source of Funding: No funding was provided for this data evaluation. All data are publicly available at www.fda.gov.; 3) Author Disclosures: The authors report no relationship or financial interest with any entity that would pose a conflict of interest with the subject matter of this article.
References: 1) Morgan Greenwald, J Ball, S Lopez, M Berg, M Greenwald. Preventive Care: Vaccines Matter. Am J Managed Care 2021; 27:294-295; 2) Drugs@FDA: FDA-approved drugs. FDA. Accessed September 25, 2020. https://www.accessdata.fda.gov/ scripts/cder/daf/; 3) Health Care Negotiation. How to achieve acceptance of medical care. Debra Cohen MD, Cynthia Leigh MD, Pratima Misra MD, Sushma Reddy MD, & Craig Sadur, MD. Developed in Concept Paper UCLA Office of Continuing Medical Education. March 19, 2021.

















































Comments (0)