More than 20% of all Americans, approximately 57 million people, consume prescription drugs intended to treat mental health issues including anxiety, depression, and panic disorders. Developing safe, targeted and effective drugs to treat these conditions has increasingly become a struggle for the pharmaceutical industry. As a result, there has been a gradual withdrawal of research dollars from this area, despite the fact that globally, the mental health pharmaceutical market is more $88 billion annually.
Until recently, most mood disorders were thought to be attributed to an imbalance of a single neurochemical agent or neurotransmitter such as serotonin. Thus, the model for treatment was based on developing drugs to raise or lower the levels of certain neurotransmitters as does the drug Prozac. However, the complexity of brain networks has proven the single neurochemical model to be an oversimplification of what is really occurring in the brain. Drugs may work to alleviate some symptoms, but they may exacerbate others. They may even contribute to new problems such as cognitive impairment, diabetes, and sometimes a decline in the condition, and even suicide.
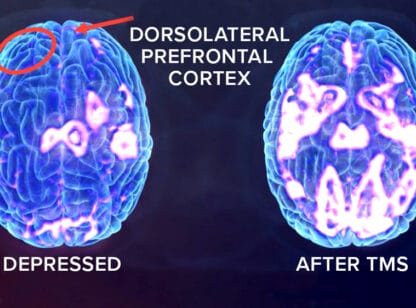
Because the diagnosis of many mental health conditions is a highly subjective process, determining the appropriate course of drug treatment is often an exercise in trial and error. Instead of focusing on single chemical neurotransmitters, mental health research is now evolving to address the brain’s functional regions known as ‘neural networks.’ These networks can be influenced using non-invasive technologies such as brain-computer interfaces (BCI) and neurofeedback or “brain training.”
A brain-computer interface is a direct communication pathway between the brain and an external device (a computer) with the purpose of assisting, augmenting or repairing cognitive and/or motor functions. Our brains produce different types of electromagnetic waves emitted at specific frequencies. These electrical events, or waves, can be detected using a set of electrophysiological sensors attached to the patient’s head. These perform a variety of brain sensing and cognitive tests after which the computer produces a detailed report on brain function and identifies any abnormalities. Based on the report of these findings as assessed by certified professionals, brain training is initiated.
Brain training is rooted in the principles of biofeedback, applied neuroscience, and evidence-based clinical practice. Through brain training, a person can learn to control the specific dysfunctional network of their brain, essentially teaching the brain to function more efficiently.
Evoke Neuroscience is a technology company that focuses on in-depth brain assessments and neurofeedback. They have produced the ‘eVox system’ which makes use of multi-modal brain evaluations that directly lead to training and rehabilitation solutions that, until recently, have not been available to the public. This system can perform a variety of brain sensing tests evoking neuropsychological assessments that can help clinicians treating disorders such as ADHD, anxiety, panic and sleep disorders. The ‘eVox system’ runs a simple and painless test that takes about 45 minutes. During the test, the patient wears an electroencephalography (EEG) cap, similar to a swim cap. The EEG cap is connected to a device that measures and then wirelessly transmits brain activity to a computer. The system then prompts the patient through a series of simple exercises on the computer.
The ‘eVox system’ reports contain objective brain maps to help develop a care plan that optimizes brain function. This new technology is advancing non-invasive options for mood disorder treatment; however, an effective plan should also address lifestyle, nutrition, stress management and psychotherapy as recommended through individual assessment.
Dr. John Dixon can be reached at the Natural Medicine Group (760) 345.7300.
Resources: 1) www.bccresearch.com/pressroom/phm/global 2) evokeneuroscience.com

















































Comments (0)