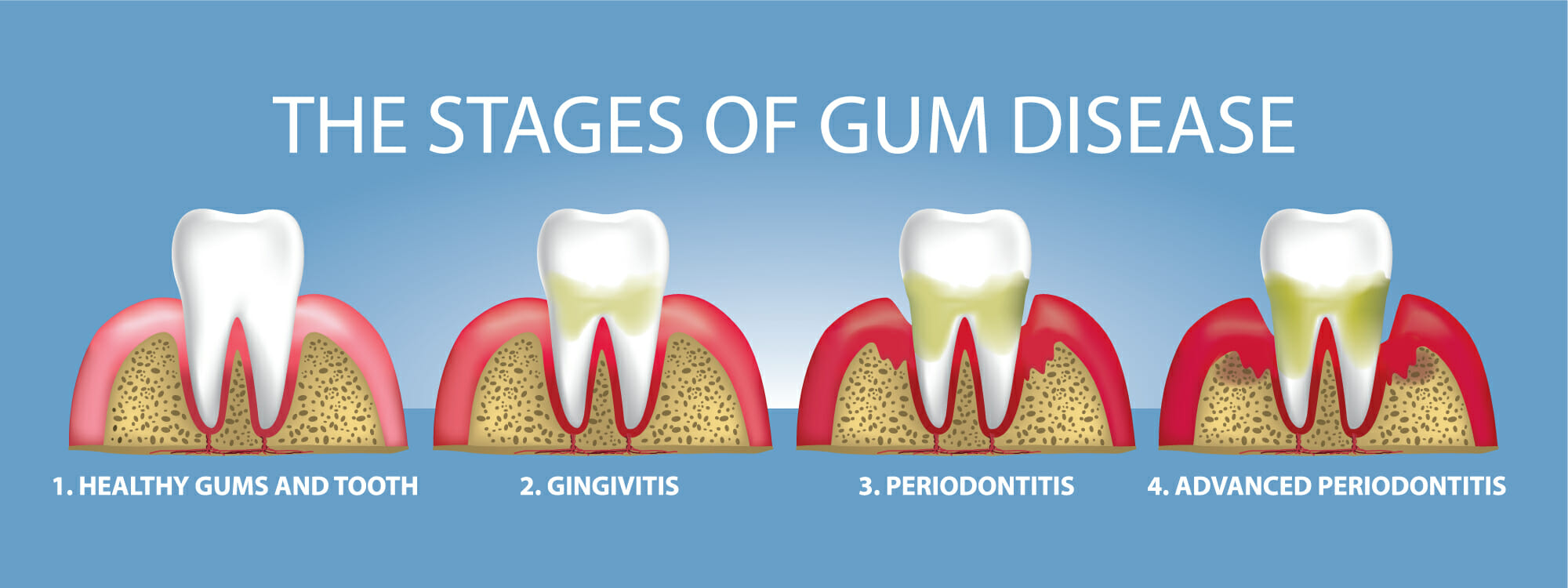
Maintaining your oral health is essential to your overall wellbeing and can help prevent pain and infections in the mouth. However, did you know that people with diabetes are at a higher risk for both early-stage gum disease (gingivitis) and advanced gum disease (periodontitis)?
Diabetes affects the body’s overall ability to process sugar. In type I diabetes, the body does not make a sufficient amount of insulin, a hormone that transports sugar from your blood to the body’s cells as needed for energy. In Type II diabetes, the body produces insulin, but the body stops responding to the insulin, which can cause a high amount of sugar reserve in the body. Both cases of diabetes result in high blood sugar levels which can cause issues throughout the body and with oral health.
Both gingivitis and periodontitis start when plaque, a soft sticky substance which is made up mostly of bacteria, gathers on your teeth. The difference between someone with diabetes, versus someone without, is the nature of the body’s inflammatory response to the oral bacteria. White blood cells in the immune system help to fight infections and bacteria in the mouth. High blood sugar can weaken those white blood cells which ultimately affects the body’s response to gingivitis and periodontal disease. Therefore, patients with diabetes may have an altered or delayed immune response.
Periodontal disease is the most common dental ailment affecting patients with diabetes. Those with uncontrolled diabetes tend to have more of an inflammatory response when presenting with periodontal disease and gingivitis, which can result in a loss of the supporting tissue and bone that make up the foundation of the teeth.
Some may not know they have diabetes, but may have one or more underlying symptoms including frequent urination, excessive thirst and more seriously, loss of consciousness if blood sugars fall too low. Untreated diabetes can also cause symptoms affecting the mouth such as dry mouth (xerostomia) caused by less salivary production; delayed wound healing, which can make one more susceptible to infections in the mouth; and cavities due to decreased salivary production and possible increase in blood sugar.
The combination of self and professional care from your dentist and physician can help keep your diabetes under control, as well as keep your smile healthy. Self-care includes avoiding smoking, controlling your blood sugar levels, properly taking prescribed diabetes medications as monitored by your physician, adopting a healthier diet and lowering sugar intake, exercising regularly, practicing proper oral hygiene and seeing your dentist for regular check-ups and cleanings. Oral treatment plans can also help decrease disease advancement.
By practicing proper oral hygiene and seeing your dentist on a regular basis, those with diabetes can maintain their optimal oral health.
Sarah Khoshniyati (“Dr. Sarah”) is a dentist with Palm Desert Smiles and can be reached at (760) 568.3602.









































Comments (0)