With the passing of Proposition 64 this past November, marijuana (aka cannabis) is now legal in California with some restrictions, depending on local and municipal guidelines. Marijuana is still considered illegal under Federal law.
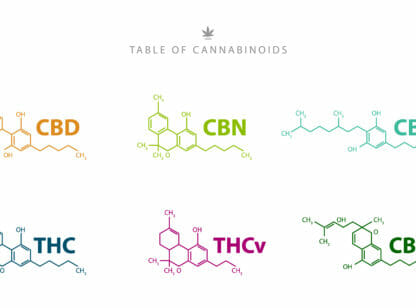
Despite records dating back 4,700 years documenting medicinal uses of marijuana, no one knew how it worked until 1964 when a researcher at Hebrew University named Raphael Mechoulam reported that one of the two main active components of cannabis was tetrahydrocannabinol (THC). This is the psychotropic and euphoric component. It is thought that THC acts on the brain by forcing itself into the intrinsic neuronal signaling system and binding tightly to specific sites in the brain. The other primary cannabinoid is cannabidiol (CBD), a non-psychotropic which means it doesn’t get you high. To date, over 483 compounds have been identified that are unique to cannabis.
Many people have questions and uncertainties pertaining to both medical and recreational uses of cannabis. In addition, a basic understanding of cannabis physiology is becoming increasingly necessary for physicians, nurses, and health care providers in providing good patient care. This understanding begins with a brief description of what is called the “endocannabinoid system.”
The endocannabinoid system is one of the most important physiologic systems involved in establishing and maintaining human health. Having the word ‘cannabis’ as part of the name of this vital system may seem confusing; however, endocannabinoids are naturally occurring chemical messengers produced by the body. They function by interacting with particular receptor sites. Endocannabinoids are literally chemical communication bridges between the body and mind. The interaction between endocannabinoids and their receptors is analogous to a lock and key mechanism; both are found throughout the body, particularly in the brain, organs, connective tissues, glands, tonsils, spleen, and immune system cells.
By understanding this system we can begin to see the basic mechanism of how all cannabinoids work. This includes marijuana and cannabis products, which are called plant cannabinoids or phytocannabinoids. The cannabinoids contained in marijuana affect human physiology because they either stimulate or down regulate the same receptors that cannabinoids produced by the body do.
The three key pieces of the endocannabinoid system are:
- The endocannabinoids, small chemical messengers that activate cannabinoid receptors. The primary endocannabinoids are anandamide and 2-AG which are naturally occurring and produced by the body.
- Cannabinoid receptors found on the surface of cells are called CB1 and CB2. CB1 receptors are one of the most abundant receptor types in the brain; CB2 receptors are more abundant outside the nervous system and found primarily in the immune system.
- Metabolic enzymes break down endocannabinoids after they are used, in particular FAAH and MAGL. Use of CBD has been shown to inhibit the FAAH enzyme and increase levels of the naturally occurring cannabinoid anandamide. This has been noted as a useful strategy in treating anxiety disorders and depression, both of which have been linked to what is called ‘endocannabinoid deficiency.’
Phytocannabinoids found in marijuana, namely THC and CBD, interact with the endocannabinoid receptors CB1 and CB2. THC, for example, gets you high because it activates the CB1 receptor in the brain. CBD can counteract some of the less desirable effects of THC, such as a tendency to produce anxiety and rapid heart rate. At the same time, CBD has many properties that THC doesn’t, such as an anti-anxiety, anti-pain, anti-psychotic and anti-inflammatory agent. Research has also shown that by adding agonists of cannabinoid receptors such as CBD, excitotoxicity, mitochondrial damage and oxidative stress can be prevented; in other words, CBD protects nerve cells against damage, degeneration, or impairment of function.
According to Dr. Ethan Russo, a noted and published cannabinoid researcher, a 1:1 mixture of THC and CBD is the best approach for treating a variety of symptoms including multiple sclerosis and many pain conditions, particularly neuropathic pain. It is his opinion that the 1:1 mixture also offers a good balance of efficacy and safety, meaning fewer side effects.
Preliminary evidence has linked genetic variations or mutations in the endocannabinoid system to specific diseases. Other studies have shown that it may be possible to predict your risk for side effects of THC such as cognitive decline, psychosis, and dependence by performing genetic testing, which is now available. This testing may also determine who will benefit from cannabinoid therapies. It should be noted that this testing is not yet FDA approved.
Dr. John Dixon can be reached at the Natural Medicine Group (760) 345.7300.
Sources: 1) https;//www.ncbi.nim.nih.gov/pmc/articles/PMC3997295/ 2) http://www.sciencedaily.com/releases/2017/07/170718142909.htm; 3) http://www.researchgate.net/publication/260760094 Care and feeding of the endocannabinoid system pharmacology of cannabinoid CB1 and CBD receptors, Pharmacol Ther. 1997; 74(2): 129-180; 4) http://www.projectcbd.org/ciencia/cannabis-pharmacology/dr-ethan-russo-cbd-clinical-endocannabinoid-deficiency; 5) Cannabinoids in neuroinflammation, oxidative stress and neurotoxicity Pharmaceutica Analytica Acta 6) Cannabinoid modulation of Neuroinflammatory Disorders, Curr Neuropharmacol 2012 Jun; 10(2) 159-166 7) Endocannabinoid System: Emerging Role From Neurodevelopment to Neurodegeneration mini Rev Med Chem 2009, Apr:9(4) 448-462.










































Comments (0)