Breast cancer steals the lives of over 40,000 people a year despite the enormous amount of new research and continued evolution of treatments. Bottom line, prevention remains the single best approach.
Regular screening for breast masses is unanimously recommended by every primary care doctor in this country. That said, the most common screening tool, mammography, is debated regarding its true benefits and limitations. Many leading physicians and medical journal publications have questioned whether mammography should be touted so highly. Since the incidence of breast cancer is not declining, are there other options that should be considered?
Some doctors choose to complement traditional mammography with Digital Infrared Thermography (IR) and genomic testing. These two relatively new testing tools give us another layer of prevention in the focus on breast cancer. Locally, accomplished surgical oncologist Philip Bretz, MD offers these tests. Dr. Bretz is the founder of the Desert Breast and Osteoporosis Institute and an acclaimed researcher in the field of breast cancer, including his current research on IR.
Dr. Bretz explains that IR combined with genomic testing has the ability to find micro breast cancers before they even have a chance to spread. Currently IR is FDA approved when used with other diagnostic modalities like mammography, MRI, or ultrasound.
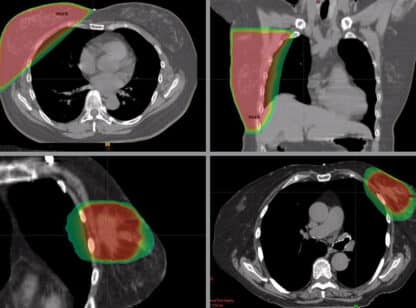
IR works both on the theory that tumors generate increased blood supply to “feed” themselves extra nutrients required in unrestrained growth. These areas will appear as thermal hot spots on the breast image. Dr. Bretz explains, “a patient gets two scores which are not subjective (an important difference from mammography and ultrasound). IR is based on military algorithms and the computer interprets the score. There are seven categories according to different regions of the breast. The overall personal score is from 1-10, and the higher your score the more abnormal the computer perceives your tissue. In addition there is the neural network score. This is a database of about 3,000 patients with a known score and tissue correlated with the score.
The advantages of Infrared Thermography are numerous. IR emits NO radiation exposure and no painful compression of the breast, and has the ability to pick up cancers as small as 4 mm. The smallest cancer that IR has detected was found a full 3 years before mammography or MRI detection.
Not everyone in the medical community agrees that IR technologies are an accurate screening tool for breast cancer, and the quality of thermal imaging cameras varies throughout the country. I look forward to the continued research in alternative screening methods such as IR and genetic testing to deepen the breast cancer detection protocol at the earliest stage possible.
For more information on IR, you can visit desertbreastinstitute.com. The doctors at Live Well Clinic utilize this screening method as part of their integrative wellness exams for women of all ages.
Dr. Nicole Ortiz is an Integrative Primary Care Doctor and co-founder of Live Well Clinic. For more info visit www.livewellclinic.org or call 760-771-5970.















































Comments (0)