About 60,000 Americans are diagnosed with Parkinson’s Disease (PD) each year. Currently, an estimated 7 to 10 million people are living with PD worldwide. This devastating disease impacts many, negatively affecting quality of life for the patient, as well as the family.
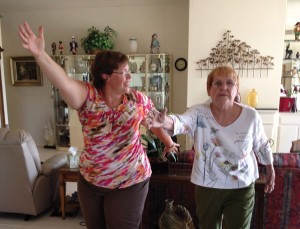
Stacy Hennis, LSVT works with a client on BIG program moves designed specifically for Parkinson’s patients
There is no cure for PD. Symptoms are standardly treated with medication to provide relief. Recent research is proving that exercise can slow or reverse some of the physical decline associated with PD. Data from the Department of Neurology at the Pittsburgh Institute for Neurodegenerative Disease, University of Pittsburgh School of Medicine, shows in animals that exercise helps to protect remaining dopamine cells by increasing GDNF, a substance important in protecting brain cells. This demonstrates that exercise can provide protection for the brain.
The George and Mary Lou Boone Center for Parkinson’s Disease Research at USC-LA has also examined the effect of exercise. They are finding changes in the excitability in the basal ganglia, an area greatly affected by PD. Researchers at the National Institutes of Health have hypothesized that exercise enhances the signals of dopamine, and improves physical function by suppressing other chemicals affecting the brain. This appears especially true after higher intensity exercise.
Exercise also helps with cerebral oxygenation–blood flow and oxygen to the brain. Aerobic exercise increases oxygen flow and leads to improved brain functioning, cognitive functioning, learning and memory, and enhanced energy levels.
It is well documented that people with PD lose muscle strength faster than other healthy adults. This leads to impaired balance and mobility. An increased risk of falls results from instability and walking difficulty. Researchers at the School of Public Health at Columbia reviewed Medicare claims and survey data. They showed a three times higher chance that someone with Parkinson’s will fall and fracture a hip as compared to their peers.
An exercise program as simple as walking can make a difference. The earlier someone starts to exercise after diagnosis, the better and longer lasting the results. Other beneficial exercise include Tai Chi, Qigong, Nordic walking (using two walking sticks), treadmill and bicycle riding. Until recently, traditional physical therapy for someone with PD focused on low to medium intensity programs and accommodations for a weakened body. A newer method is the LSVT® BIG program, an innovative treatment that focuses on big movements, while addressing the sensory problems that exist with PD. For example, someone with PD may feel that they are walking normally when they’re actually taking small steps or shuffling. LSVT® BIG takes PD symptoms into consideration, and can only be provided by a LSVT® certified physical or occupational therapist.
Please remember to always seek your physician’s approval before beginning an exercise program.
Stacy Hennis is the owner of New Beginning Physical Therapy, Inc., an in-home therapy company. She has a Masters degree in Physical Therapy, as well as advanced certifications in treating adults with stroke, brain injuries and Parkinson’s. Stacy can be reached at 760-218-9961 or online at NewBeginningPT.com.






































Comments (0)