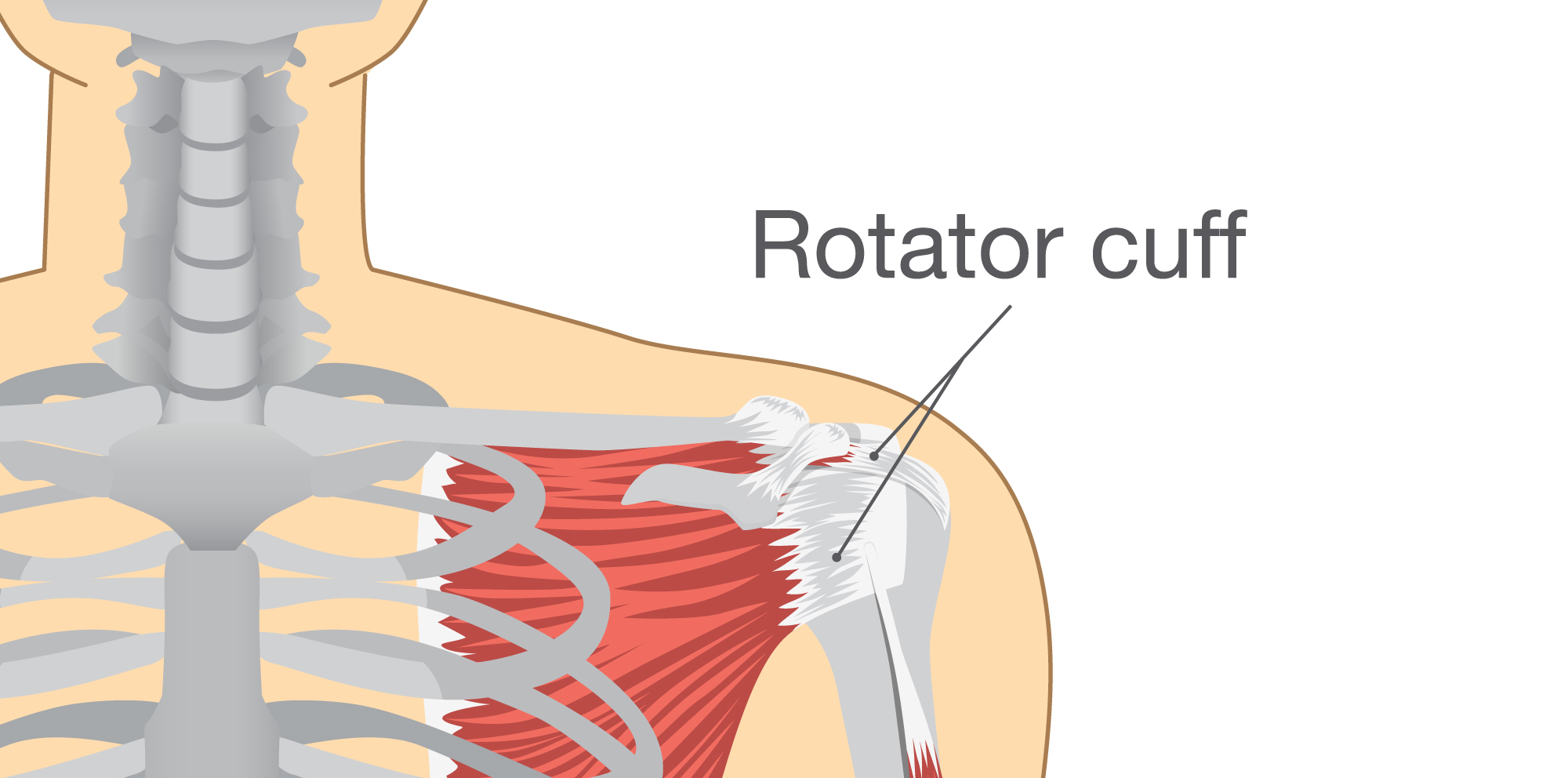
The rotator cuff, despite the name, is not a single structure but a group of muscles and tendons.
Certain jobs and sports increase the risk of rotator cuff injuries, as does increasing age. When I see a rotator cuff injury, I’m glad that I can offer a variety of treatment options to help patients get back to the activities they need, or like, to do.
Let’s start with a little anatomy
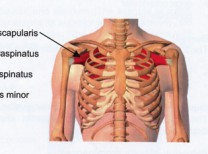
The shoulder is a ball-and-socket joint composed of the upper arm bone (humerus), shoulder blade (scapula) and collarbone (clavicle). Four muscles and their associated tendons make up the rotator cuff. The supraspinatus muscle runs over the top of the shoulder. The subscapularis muscle covers the front of the shoulder and part of the upper chest. In the back of the shoulder, the infraspinatus muscle runs from the top of the shoulder down to the edge of the scapula. The teres minor muscle attaches slightly below the infraspinatus and runs under it to the bottom edge of the scapula. These muscles attach the humerus to the scapula, keep the head of the humerus in your shoulder socket and allow you to lift and rotate your arm.
Risk factors for rotator cuff tears
Genetics. These injuries tend to run in families, which indicates there may be a genetic component.
Repetitive arm movements. Throwing is one of the classic risk factors for rotator cuff injury; baseball pitchers, for example, often develop rotator cuff problems. Archery, volleyball, and tennis can also put stress on the shoulder joint and increase the risk of a rotator cuff problem.
Certain jobs. Any job in which the shoulder joint gets a workout can contribute to rotator cuff problems. Overhead painting or carpentry both require repetitive arm motions.
Increasing age. Most of the rotator cuff tears I see are in people over the age of 50. This is pretty much a matter of wear and tear on the shoulder joint, which can be exacerbated if the individual has a job or plays a sport that also increases the risk or a rotator cuff problem. The tendons have less blood supply as we get older, which makes them more prone to injury. Older people are also more likely to develop bone spurs in the shoulder, which can rub on and damage the tendons.
Rotator cuff symptoms
Common symptoms of a rotator cuff injury include the following:
Pain: a dull ache deep in the shoulder is more common in rotator cuff problems that result from overuse or repetitive motion. An injury such as a fall can cause acute, severe pain.
Difficulty sleeping: pain in the shoulder can result in an inability to sleep on the affected side.
Functional impairment: difficulty performing actions like combing your hair and reaching behind your back or overhead.
Joint noise: the shoulder may have a crackling sound when you move it or place your arm in certain positions.
Weakness: arm weakness may occur in some cases.
When I see symptoms that indicate a possible rotator cuff injury, I will usually order X-rays as well as a magnetic resonance imaging (MRI) test. The X-rays will show arthritis or the presence of bone spurs, while the latter two are better for finding soft tissue injuries and actual tendon tears.
Treatment options
Luckily, in about 80 percent of people who have a rotator cuff injury, rest, over-the-counter medication, activity modification and physical therapy can resolve the problem and prevent further injury. If not, the next thing I typically recommend is a steroid injection to relieve pain and inflammation. However, if you have a large tear, your symptoms don’t diminish over time or you have significant weakness and loss of function in the shoulder, surgery may be the best choice.
Surgery can often be performed with an arthroscope – a special device with a tiny camera that allows for a couple of small incisions and minimal tissue trauma. Arthroscopic surgery can include stitching a torn tendon, debriding (removing) frayed tissue or reattaching the tendon to bone. If you have a large tear, bone spurs or considerable damage to the rotator cuff, you may need a longer recovery time. Arthroscopic surgery can often be performed on an outpatient basis.
Recovery and rehabilitation
The recovery period after surgery will vary according to the severity of the original problem and the type of surgery needed. You can certainly expect pain and discomfort in the first week, although that will gradually diminish. However, it’s likely to take several weeks or months for full recovery. In all cases, physical therapy is necessary to prevent the shoulder from becoming stiff and to strengthen the muscles. Physical therapy also stretches muscles so you will still have good range of motion. Your active participation in the rehabilitation process will help shorten the recovery time and increase your chances of a good outcome. However, overdoing it can cause a setback, so always follow your doctor and/or physical therapist’s recommendations and instructions.
Staying healthy
A functional shoulder is necessary for many work activities as well as many of the recreational activities we can enjoy in our desert locality. Rotator cuff injuries can make it difficult to lift or push at work. If you like to swim, play tennis, volleyball or golf, a rotator cuff injury can limit your activity or even force you to stop playing entirely. Even walking or hiking can be uncomfortable when your shoulder hurts all the time. It’s also difficult to exercise the upper body when the rotator cuff has been injured, which means your overall health may suffer.
Although there is no guarantee, daily shoulder stretches and regular strengthening exercises may help prevent rotator cuff injuries in some cases. The focus of the exercise should be on the muscles in the back of the shoulder and around the shoulder blade. A physical therapist or qualified exercise trainer can help create an exercise program that will achieve your goals. If you have shoulder pain that won’t go away, however, it’s a good idea to consult a doctor.
Dr. Sydney Pardino is an orthopedic physician with a private practice in Palm Desert. He can be reached at (760) 340.6784 or visit www.cuttingedgeortho.net








































Comments (0)