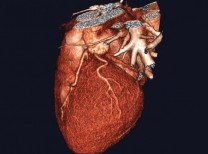
Atrial fibrillation (A-tre-al fi-bri-LA-shun), or “A-Fib,” is a problem with the heart’s electrical system which causes the heart to beat too fast, too slow, or with an irregular rhythm.
While many may consider their fluttering heart a strange but passing sensation, heart palpitations, coupled with dizziness and shortness of breath, are cause for concern. By pumping blood through your heart irregularly, and not getting enough oxygen to the body, A-Fib can lead to heart and valve diseases, anxiety, and chronic fatigue. More serious conditions include congestive heart failure and stroke.1
Although A-Fib can occur at any age, the risk increases as you get older. Approximately 2.5 million Americans are affected, and that number is expected to increase with our aging population.2
If A-Fib goes untreated, you are five-to-six times more likely to have a stroke than the general population.3 And the condition is responsible for up to 25% of all strokes.4
“A-Fib may happen rarely or every now and then, or it may become an ongoing or long-term heart problem that lasts for years,” explains Hetal Bhakta, MD, an electrophysiologist (heart rhythm disorders specialist) at Desert Regional Medical Center. “Fixing it before it progresses is the key.”
Dr. Bhatka compares the condition to the wiring in your home. “Your heart has four chambers, like rooms in your house. Within the walls of your house, you have the plumbing, electrical, etc. A house that was built 50-60 years ago has more wear and tear than a house built ten years ago. If one day you enter a room and try to turn on the lights in that old house and they flicker, you know you have a small electrical problem to fix.” He compares this to episodes when you are going in and out of A-Fib. “Now if you don’t fix that electrical short, then next time, the lights may not turn on at all because that short has progressed and damaged additional electrical wiring.”
Bhatka indicates that when the disease is addressed early, areas of concern can be isolated and all the other wiring in the heart can be left alone to operate as is. “If you don’t, in years to come, you may find that the whole wiring system is damaged and your treatment options are limited.”
How is A-Fib detected?
“If a patient comes to us with concerns about their heart rate, we use a Holter monitor (a small wearable device that records heart rhythm) for a recommended duration ranging from 24 hours up to one month,” says Bhatka. “Patients can press a button when they feel symptoms and we can review the heart’s activity at that specific time. If the activity is normal, then something else is causing the symptoms, but if the heart is irregular, then we have identified the problem and further examine the extent.”
Treatment options
Treatment for A-Fib depends on how often you have symptoms, how severe they are, and whether you already have heart disease. General treatment options include medicines, medical procedures, and lifestyle changes. The primary goals of treatment are to prevent blood clots from forming, thus lowering the risk of stroke; controlling heart rate; restoring a normal heart rhythm; and treating any underlying disorder that’s causing or raising the risk of A-Fib.5
Bhatka states that the first treatment option is often cardioversion (or electric shock) that resets the heart “like a reboot on the computer.” Sometimes this is coupled with medication that soothes the heart and maintains a consistent rhythm. The longer one waits the less effective these treatments are.
If A-Fib reoccurs, the next step is usually endovascular or catheter ablation surgery which targets the specific faulty circuits in the heart and ‘scars’ the tissue to keep it from doing further damage. This procedure can be compared to a stent operation and is less invasive than the third option which is cardiothoracic (or open heart) surgery.
Treating underlying causes and reducing risk factors
There are many conditions known to raise the risk of A-Fib, such as high blood pressure, high cholesterol, hyperthyroidism (too much thyroid hormone), obesity, diabetes, and lung disease. Managing these conditions is an important part of treating A-Fib. Research also suggests that high-dose steroid therapy, such as for the treatment of asthma and other inflammatory conditions, may act as a trigger in people who have other A-Fib risk factors.5
Certain lifestyle factors can raise your risk for A-Fib as well. For example, drinking large amounts of alcohol, especially binge drinking, raises your risk. Even modest amounts of alcohol can trigger the disease in some people, as can caffeine or psychological stress. Moderating alcohol intake, following a healthy diet, cutting back on salt intake (to help lower blood pressure), quitting smoking, and reducing stress are recommended.
So when do you know if it is a passing flutter or A-Fib? “If heart palpitations or irregular heart beats are occurring frequently or concerning you, then it is worth checking out,” advises Bhatka. “By understanding atrial fibrillation, you can better care for your heart, and work with your health care provider in managing your heart health.”
To reach Dr. Bhakta, or for a free referral to another physician, call Desert Regional Medical Center’s referral line at 800-491-4990. Please mention that you read this article in Desert Health.
References: 1) National Institutes of Health; 2) Go AS. “Prevalence of Atrial Fibrillation in Adults: National Implications for Rhythm Management and Stroke Prevention: The Anticoagulation and Risk Factors in Atrial Fibrillation (ATRIA) Study.” Journal of American Medical Association. May 9, 2001-Vol 285, No. 18.; 3) Gillinov AM, Blackstone EH, et al. “Atrial Fibrillation: Current surgical options and their assessment.” Ann. Thorac. Surg. 2002; 74:2210-17.); 4) Andy C. Kiser, MD., FirstHealth Arrhythmia Center, Pinehurst, NC. http://www.convergentprocedure.com/total-solution.htm); 5) www.stopafib.org









































Comments (0)